6 min read
Measuring the Cost of Denials and the Impact of Prevention
By: Lori Zindl on Aug 23, 2021 10:07:36 AM
When it comes to denial management, there is no “one-size-fits-all” approach.
Different organizations use different systems, departments, metrics, third-party vendors, and technology to guide and manage their approach to denials. As technology and data-tracking capabilities have advanced, however, denial prevention has risen to the forefront as a strategy that not only addresses denials but prevents them from happening in the first place.
Unfortunately, however, far too many healthcare organizations are still using the traditional “follow-up method” of denial management, in which claims are moved quickly through the process and onto the payer as fast as possible.
These providers zero in on their clean claim rate (percent of claims not stopped by internal edits before submission) as the most important indicator of success and simply wait for the payer to tell them what’s wrong with each claim.
Although these providers may have a spectacular clean claim rate, their rate of denials can still be astronomical because their denial management efforts happen on the back end once claims have already been denied.
As a result, claim denials continue to increase along with the cost to collect and the length of the payment cycle.
This article aims to quantify the cost of denials and give organizations an actionable roadmap for denial management that is based on data and prevention rather than follow-up and reactivity.
One Size Fits All?
In an effort to aid in denial management efforts and help standardize the way healthcare organizations measure and talk about denials, HFMA developed the “Claim Integrity Task Force.” The group ultimately identified and defined 6 key performance indicators (KPIs) to be used for measuring the outcome of denial management efforts.
- Initial denial rate (as a percentage of volume and dollars)
- Primary denial rate
- Denial write-offs as a percentage of net patient service revenue
- Time from initial denial to appeal
- Time from initial denial to claim resolution
- Percentage of initial denials overturned (with reference to charges, volume, and inpatient denials that converted to observation)
Notably Clean Claim Rate didn't make the list.
Instead, the task force included initial denial rate (percent of claims denied upon first submission) as the first metric on the list. Experts recognize that claims paid on first submission save you money, time, and resources spent on costly re-work and appeals.
This is precisely why we consistently measure our clients’ first pass yield. Similar to HFMA’s Initial denial rate (% of claims denied upon first submission), efficientC’s First Pass Yield rate measures the percent of claims paid on first submission.
The Cost of Denials
Why is it so important to understand how many claims are actually being paid upon first submission?
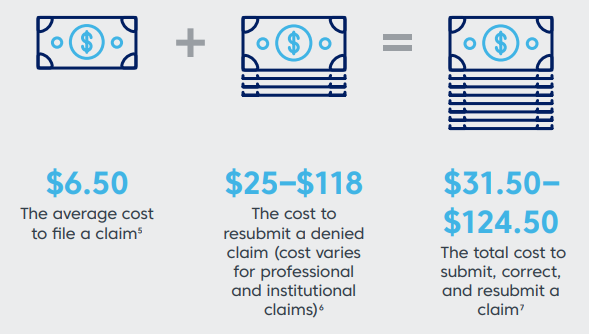
Because each denied claim is costing your organization money. In fact, a 2017 Change Healthcare analysis found that each denied claim costs on average $117. Some other sources have estimated that this number is closer to about $25 per claim, which may be more realistic for professional claims in a smaller practice setting.

Image Source: Change Healthcare Infographic
Additionally, Change Healthcare states that 65% of denied claims are never resubmitted, which indicates that organizations are also experiencing large amounts of lost revenue due to denials. Industry sources also suggest that almost 60% of claims rebilled after a denial will deny again.
Let’s take a look at an example. If the cost of denials at XYZ Healthcare is around $75 per denied claim, and they submit 20,000 claims per month, it is likely that around 4,000 of those claims will deny (based on a 20% initial denial rate).
This amounts to a cost of about $300,000 every month or $3.6 million in a single year!
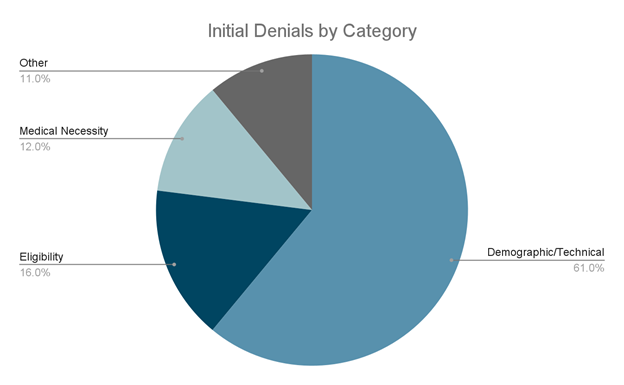
Now if your organization has chosen to focus on prevention over follow-up, there’s good news for you. 90% of denials are preventable and occur most often in categories like medical necessity, eligibility, and demographic or technical errors.
Financial Impact of Denial Prevention
If XYZ Healthcare from the example above can implement an effective denial prevention program and reduce its initial denial rate from 20% to 10%, what would be the financial impact?
The organization’s total denied claims per month would fall to 2,000, representing an estimated cost savings of $150,000 each month. Said another way, every additional claim that is paid upon first submission becomes first pass reimbursement. This improves the organization’s cash flow, reduces revenue leakage, shortens the payment cycle, and even boosts patient satisfaction.
Implementing a Successful Denial Prevention Strategy
In an effective denial prevention program, every effort is made to prevent denials prior to billing. For example, edits built into the claim scrubber can stop at-risk claims before they result in denials. While this step does require a biller to clear the edit, stopping to make the necessary changes prior to billing keeps the payment cycle short.
If the claim is stopped on day 1, it can be fixed and rebilled on day 2 and paid on day 16 or 17.
Another part of prevention is looking at data trends and implementing process changes, edits, or change routines:
- If a large portion of total claim denials stem from medical necessity issues, how can your organization proactively address that? Is clinician education needed to ensure clinical documentation includes all necessary details?
- If denials stem from front-end errors related to demographic information or eligibility, how can processes be improved to ensure this information is captured accurately and completely? Is training needed for front-end staff?
Organizations who pay close attention to this type of denial data can nimbly pivot to address the root cause of denials in any area. Then, by continuing to monitor performance, leaders can determine whether the changes made are actually resulting in fewer denials.
Bottom line: top-performing organizations are getting claims paid in 20 days or less. That number indicates many claims are are being paid on first submission, which hinges on a strong denial prevention strategy.
Start by getting on the same page as your claims management partner. Denial prevention should be top of mind, with the ultimate goal of stopping claims before they are denied in order to shorten the payment cycle, improve cash flow, reduce write-offs and revenue leakage, and reallocate billing office resources that were previously dedicated to denial follow-up.
Are you looking for a claims management partner who can deliver in this area? We would love to talk with you. efficientC is a denial prevention platform, designed to STOP and FIX claims prior to billing.
On average, our clients see 90%-95% of claims paid within 20 days, a 15% overall improvement in cash flow, and a 40% reduction in denials after just 60 days.
The results speak for themselves. If your organization makes the move to efficientC, your total cost of denials will go down. Whether this is through a reduction in A/R days or an improved overall payment rate, the difference is significant.
You can get in touch with a member of the efficientC here.
Do not forget to subscribe to Revenue Cycle Matters for healthcare billing best practices and industry tips!
Related Posts
What's Eating Your Bottom Line: The True Cost of Denials
The Medical Group Management Association (MGMA) has estimated the average cost to rework a claim at...
No Denials Tool in Place Means Opportunity for Improvement
A recent study released by HIMSS Analytics found that 31% of providers do not have a formal denials...
Expect More from Your Clearinghouse - The efficientC Difference
As a healthcare leader in 2020, your bottom line is largely dependent on your ability to get claims...
